Table of Contents
The immune system shields the body from a range of pathogens and the toxins. Innate immunity is the first line of defense against pathogens via physical and chemical barriers , such as mucus layers, skin and saliva. The second line of defense is also triggered by innate immunity via the phagocytes. This defense line is triggered via adaptive immune system. Passive and active immunity are two forms of adaptive immunity. Both types of immunity work with antibodies. The primary distinction between passive and active immune systems is the fact that active immunity gets cultivated through the creation of antibodies in the person’s body, while passive immunity is triggered by antibodies created in the outside.
What is Active Immunity?
Active immunity is an immunity that results from the production of antibodies in the body’s immune system as a response direct contact with an antigen. The two types of active immunity are naturally-acquired active immunity and artificially-acquired active immunity. When you acquire active immunity naturally, the body’s natural exposure to antigens. The surface molecules of an antigen act as epitopes to facilitate the creation of antibodies. T cells (cytotoxic T cells and helper T cells) Antigen-presenting cells (dendritic cells and macrophages) B cells (memory B cells and plasma B cells) are involved in the natural acquisition of active immunity. Because the immune system of the body generates antibodies on its own and it takes time to develop natural-acquired active immunity.
During artificially-acquired active immunity, the antigens are artificially introduced into the body in the form of vaccines. The immune response that occurs after the initial contact with the pathogen can be known as the primary response. The second response takes place after the second exposure to the pathogen and triggers a more robust immune response. Through the generation by memory cells the active immunity lasts for a long period of duration.
What is Passive Immunity?
Passive immunity is a temporary immunity that results from the induction of antibodies from outside. This means that passive immunity doesn’t require immediate exposure of the body to pathogens. Because that antibodies enter the human body this immune response can be produced quickly. However, passive immunity lasts for a few days.
Passive immunity can be two types; naturally-acquired passive immunity or artificially-acquired passive immunity. The passive immunity that is acquired naturally involves the transfer of antibodies from the mother to the baby through breast milk and colostrum. Artificially-acquired passive immunity is the injection of antisera and the injection of snake antivenom.
Similarities Between Active and Passive Immunity
- Active and passive immunity can be described as two kinds of adaptive immunity.
- Both passive and active immunity work with antibodies.
- Both active and passive immunity can be either naturally-acquired or artificially-acquired.
Differences between Active Immunity and Passive Immunity
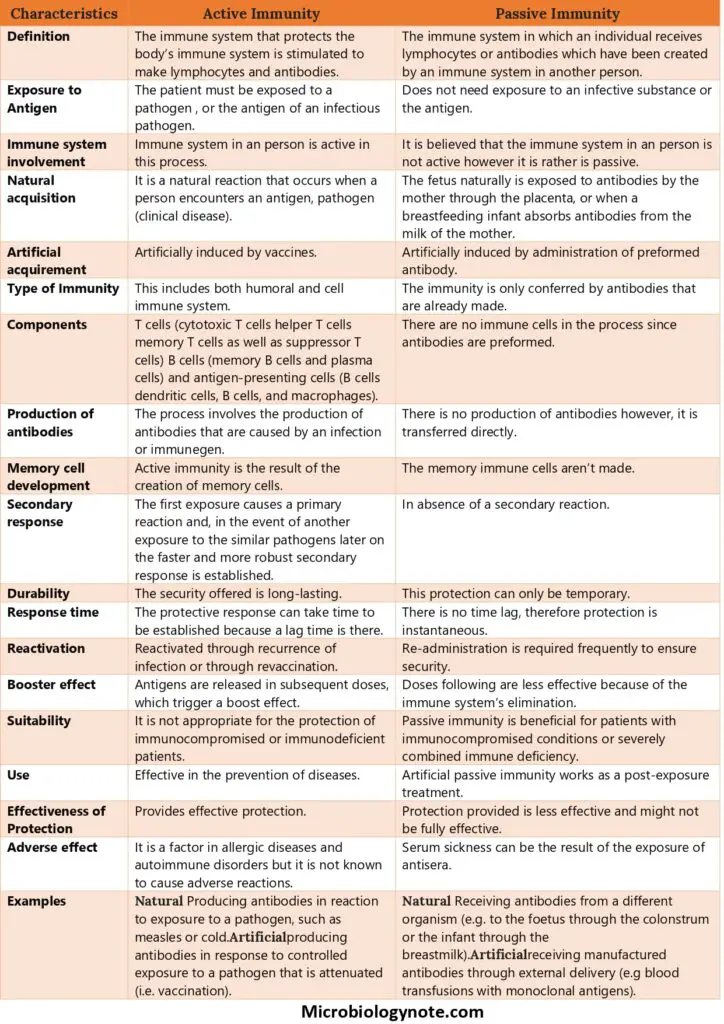
| Characteristics | Active Immunity | Passive Immunity |
| Definition | The immune system that protects the body’s immune system is stimulated to make lymphocytes and antibodies. | The immune system in which an individual receives lymphocytes or antibodies which have been created by an immune system in another person. |
| Exposure to Antigen | The patient must be exposed to a pathogen , or the antigen of an infectious pathogen. | Does not need exposure to an infective substance or the antigen. |
| Immune system involvement | Immune system in an person is active in this process. | It is believed that the immune system in an person is not active however it is rather is passive. |
| Natural acquisition | It is a natural reaction that occurs when a person encounters an antigen, pathogen (clinical disease). | The fetus naturally is exposed to antibodies by the mother through the placenta, or when a breastfeeding infant absorbs antibodies from the milk of the mother. |
| Artificial acquirement | Artificially induced by vaccines. | Artificially induced by administration of preformed antibody. |
| Type of Immunity | This includes both humoral and cell immune system. | The immunity is only conferred by antibodies that are already made. |
| Components | T cells (cytotoxic T cells helper T cells memory T cells as well as suppressor T cells) B cells (memory B cells and plasma cells) and antigen-presenting cells (B cells dendritic cells, B cells, and macrophages). | There are no immune cells in the process since antibodies are preformed. |
| Production of antibodies | The process involves the production of antibodies that are caused by an infection or immunegen. | There is no production of antibodies however, it is transferred directly. |
| Memory cell development | Active immunity is the result of the creation of memory cells. | The memory immune cells aren’t made. |
| Secondary response | The first exposure causes a primary reaction and, in the event of another exposure to the similar pathogens later on the faster and more robust secondary response is established. | In absence of a secondary reaction. |
| Durability | The security offered is long-lasting. | This protection can only be temporary. |
| Response time | The protective response can take time to be established because a lag time is there. | There is no time lag, therefore protection is instantaneous. |
| Reactivation | Reactivated through recurrence of infection or through revaccination. | Re-administration is required frequently to ensure security. |
| Booster effect | Antigens are released in subsequent doses, which trigger a boost effect. | Doses following are less effective because of the immune system’s elimination. |
| Suitability | It is not appropriate for the protection of immunocompromised or immunodeficient patients. | Passive immunity is beneficial for patients with immunocompromised conditions or severely combined immune deficiency. |
| Use | Effective in the prevention of diseases. | Artificial passive immunity works as a post-exposure treatment. |
| Effectiveness of Protection | Provides effective protection. | Protection provided is less effective and might not be fully effective. |
| Adverse effect | It is a factor in allergic diseases and autoimmune disorders but it is not known to cause adverse reactions. | Serum sickness can be the result of the exposure of antisera. |
| Examples | Natural Producing antibodies in reaction to exposure to a pathogen, such as measles or cold.Artificialproducing antibodies in response to controlled exposure to a pathogen that is attenuated (i.e. vaccination). | Natural Receiving antibodies from a different organism (e.g. to the foetus through the colonstrum or the infant through the breastmilk).Artificialreceiving manufactured antibodies through external delivery (e.g blood transfusions with monoclonal antigens). |