Advertisements
Table of Contents
What is Immune Response?
- Immune Response is the mechanism through which the host’s immune system reacts to a damaging foreign particle or pathogen (antigen) in the body.
- It involves identifying the antigen and activating defence mechanisms against invading infections.
- Antigens are chemicals that are located on the surface of cells, viruses, bacteria, or fungi, and immune responses are elicited in order to protect against them.
- Antigens in nature are mostly proteins, but they can also be medications, poisons, toxins, and foreign particles such as splinters.
- Inducing an immune response are pathogens such as bacteria, viruses, fungi, and parasites.
- Therefore, the immune system plays a crucial role in identifying and killing or attempting to destroy antigen-containing compounds.
- Immune responses to antigens can be classified as either primary or secondary. The main immunological response of the body to antigen happens the first time it encounters the antigen.
- Depending on the type of the antigen and the location of entry, this reaction can take up to fourteen days to resolve and results in the production of memory cells with a high level of antigen specificity.
- The humoral response, which is mediated by B cells with the assistance of T cells, creates antigen-specific antibodies with high affinity.
- In contrast, the CD8 T-cell response generates enormous numbers of antigen-specific lymphocytes capable of directly destroying infected cells.
- Upon antigenic stimulation, antigen-specific CD4 T cells, which feed B cells with cytokines and other stimulatory substances, can also proliferate.
- Following a second encounter with the same antigen, the secondary response of both B- and T-cells is more fast, resulting to the activation of previously produced memory cells. This response differs quantitatively and qualitatively from the initial response.
What is Primary Immune Response?
- Primary immunological reaction refers to any immune response of the immune system that includes antibody and/or cell-mediated immunity generation. It follows the initial encounter with a foreign antigen.
- At the commencement of the initial immune response, no antibodies have been previously created.
- Thus, naive B cells are activated and differentiated into plasma B cells that produce antibodies. Some B cells differentiate into memory cells.
- The lag phase, i.e. the period of time during which antibodies are generated against a specific antigen, is lengthy in the main immunological response.
- Occasionally, the lag phase can last for weeks or even months.
- In the first immune response, the amount of antibodies generated or antibody titre is modest. IgM is the predominant antibody generated during the initial immune response. The antibody titer becomes undetectable over time.
Mechanism
- Memory B-cells are plasma cells with a lengthy life span that are primarily generated in the germinal centres.
- During the initial phase of the main immune response, T-cells stimulate naive B-cells. B-cells then migrate to secondary lymphoid organs such as the spleen and lymph nodes, where they enter B-cell follicles or germinal centres in the cortex.
- B-cells proliferate and undergo somatic hypermutation within the germinal centre, which modifies their receptor’s affinity. The receptors’ affinity within the germinal centre is then evaluated.
- B-cells that can bind their antigens to follicular dendritic cells receive survival signals from T-cells, whereas those that cannot bind or bind with a lower affinity are outcompeted and undergo apoptosis. In addition, B-cells can class flip from IgM to IgA or IgG antibodies.
- B-cells differentiate into plasma cells and memory B-cells following somatic hypermutation and class transition. Following the initial immunological reaction, plasma cells are short-lived and perish fast.
- Memory cells, on the other hand, are long-lived and migrate to the periphery, where they are more likely to meet antigen upon re-exposure. Many of the circulating B-cells become concentrated in Peyer’s patches and other locations of the body with a high likelihood of antigen contact.
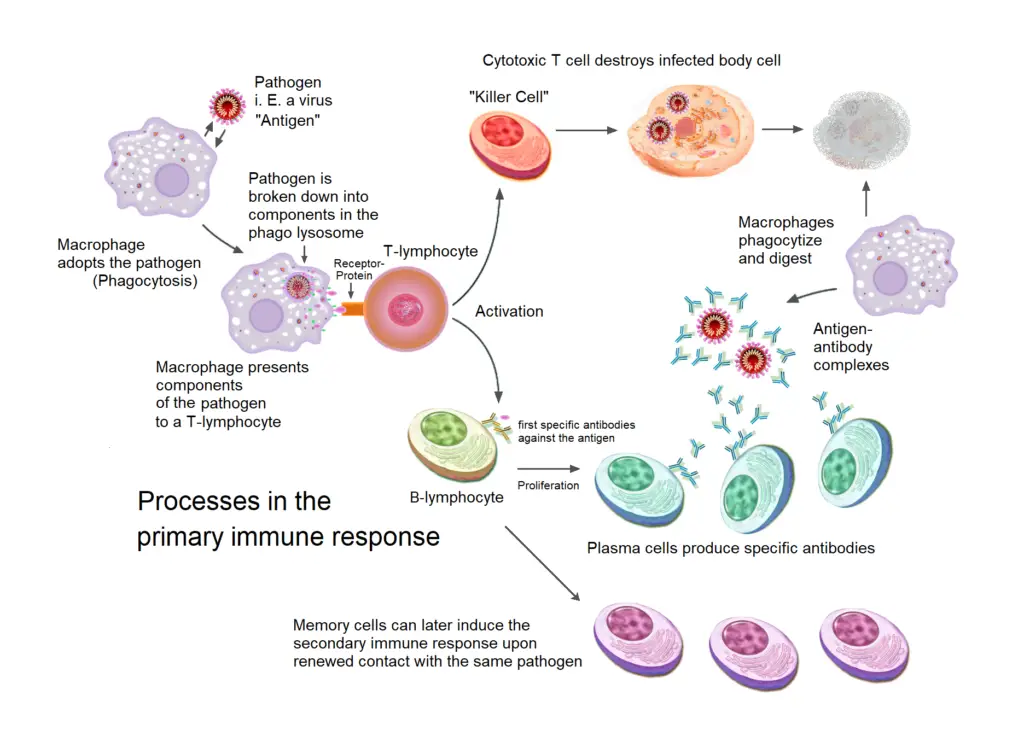
Stages of Primary Immune Response
When an individual is exposed to an antigen for the first time, an initial immune response that is very transient and feeble occurs. This can be separated into four phases: lag, exponential, steady state, and decline.
Lag (latent) phase
- It takes roughly a week between initial antigen exposure and the detection of antibodies in the blood.
- During this period, specialised B and T lymphocytes are activated by antigen interaction.
Exponential phase
- Here, the levels of antibodies, which are released by a vast number of plasma cells, grow sharply (differentiated B cells).
Steady state (plateau) phase
- Due to the ongoing release of antibodies to replace those that have degraded, antibody levels remain relatively constant.
Declining phase
- Existing plasma cells die, and no new plasma cells are produced to replace them, causing a gradual decline in antibody levels.
- Immunogen has likely been removed from the body; hence, no more antibody synthesis is required.
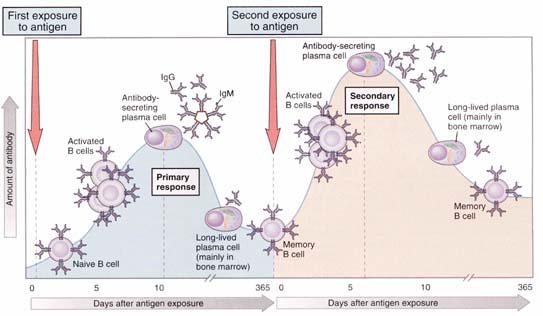
What is Secondary Immune Response?
- For future contacts with identical antigens, secondary (anamnestic) immune responses are triggered.
- In this instance, the lag phase is shorter, and high and stable quantities of antibodies are produced in a matter of days. This is because antigen-specific memory T and B cells were initially generated during the primary immune response.
- Due to the rapidity of the secondary immune reaction, the antigen can be cleared from the body shortly after it enters, before it can cause disease.
- To ensure that the virus has been eradicated, the antibodies produced remain in circulation longer.
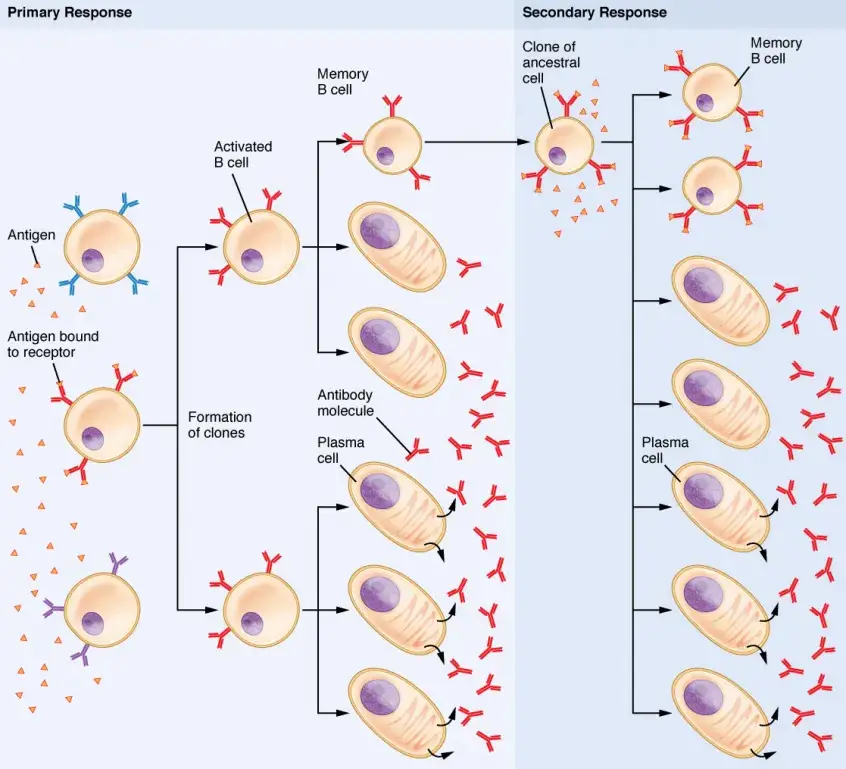
Mechanism
- When these memory cells re-encounter their unique antigen, they multiply rapidly and develop into plasma cells.
- These plasma cells subsequently produce an abundance of antibodies to eliminate the antigen.
- A minority of these memory cells may also enter germinal centres for class switching and affinity development.
- By displaying antigen on MHC-II molecules, memory B-cells can also activate effector T-cells.
- Memory B-cells undergo plasma cell development more rapidly than naive B-cells. Memory cells can endure for decades, allowing them to respond to many stimuli over time.
- In addition, they do not require constant interaction with antigen or T-cells in order to live. In response to antigen, cells that have previously undergone class switching and affinity maturation can proliferate more rapidly and make antibodies with a higher affinity, such as IgG.
Factors that Influence the Type of Immune responses
- Type of antigen- Primary immune immune responses are triggered by interaction with any form of antigen, whereas secondary immune responses are triggered by interaction with protein antigens.
- Route of antigen entry – The initial immune response to an antigen is regulated by the antigen’s route of entry. i.e., entry through the bloodstream, which evokes an immune response in the spleen, or entry through the skin and subcutaneous tissue, which elicits an immunological response in the nearby lymph nodes. Thirdly, antigens can enter the body through mucosal surfaces, such as the gastrointestinal, pulmonary, and reproductive tracts, triggering an immune response in the submucosal lymphoid tissues.
- Antigen-presenting cells – Antigens are processed by dendritic cells, macrophages, and B-lymphocytes, with dendritic cells being the most efficient. Dendritic cells are mostly responsible for conveying processed antigens to T-cells in primary immunological responses, where they play a vital role in antigen interaction. B-cells perform well as antigen-presenting cells during secondary immune responses. Antigen-processing and presentation are phagocytic mechanisms that present an antigen broken down into peptides in conjunction with the Major Histocompatibility Complex (MHC).
- Antigen Receptors – Antigen interactions with immune cells, particularly B and T-cells, are mediated by these cells’ ability to identify them (antigens). B-cells have B-cell Receptors (BCR), also known as immunoglobulins, to which antigens bind, whereas T-cells must identify antigens that have been processed and joined to MHC complex molecules in order to bind to T-cell Receptors (TCR).
- Antigen Complexity- Complexity of Antigens Antigens come in a variety of sizes and forms, and the antigen determinants are known as epitopes. These epitopes must be identified by both T- and B-cells and elicit an immunological response in order to activate B-cells, which then pass through the thymus and activate T-cells. Some antigens, however, are not immunogenic and hence require a carrier protein such as immunoglobulin in order to be immunogenic and elicit an immune response.
- In addition to clonal expansion, affinity maturation, class switching, and memory cells, other factors that determine the kind of immune response are clonal expansion, affinity maturation, and memory cells.
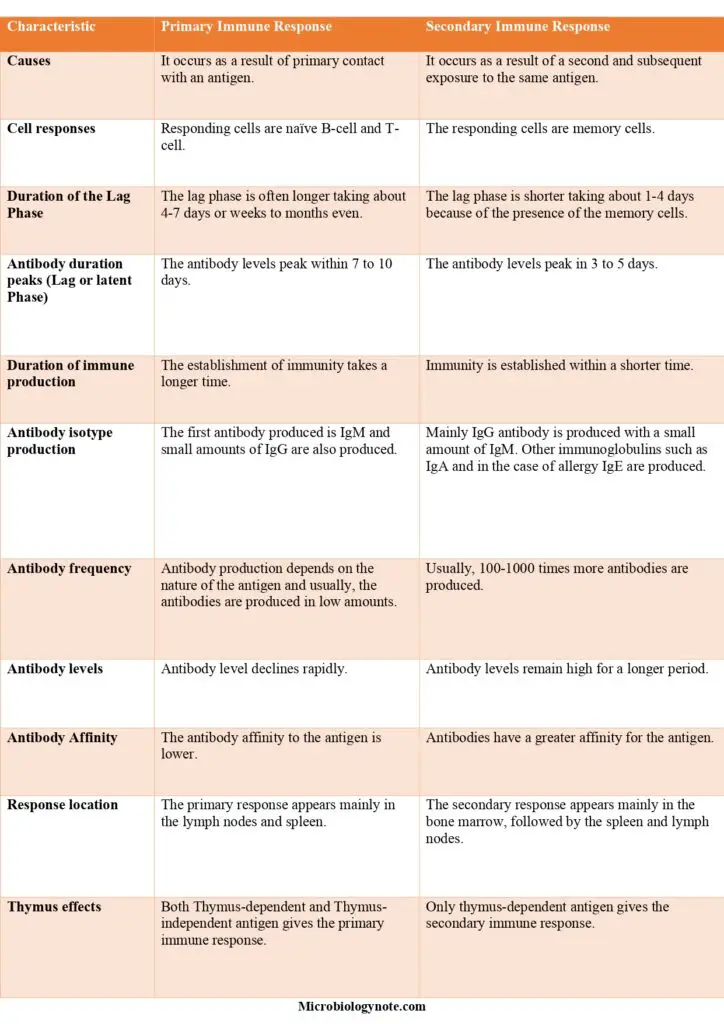
Difference Between Primary Immune Response and Secondary Immune Response
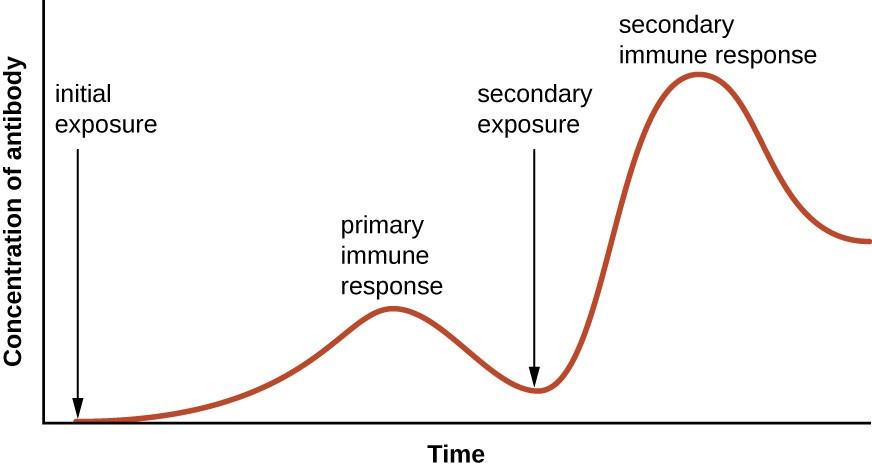
- Normally, it takes a few days for the first antibody response produced by the first exposure to thymus-dependent antigens to become evident as a circulating antibody. The term “lag phase” describes this type of delay. It is conditional on many variables, such as the antigen’s type, the immunisation route, the dosage, and the species receiving the vaccine.
- Low-affinity IgM and high-affinity IgG antibodies are found initially, with the latter being more common when the antigen persists. After a while, antibody levels drop if the body isn’t constantly being challenged by new antigens.
- A rapid secondary antibody response was elicited in response to a second exposure to the thymus-dependent (TD) antigen. This causes the formation of memory cells to stem directly from the main reaction.
- The secondary response is typically more rapid, substantial, and long-lasting than the initial one.
- Antibodies with higher affinity are formed in the secondary immune response, and IgG or IgA antibodies predominate depending on the region of antigen reaction. Because the antigen attaches so tightly to the antibody, this happens.
- Immune defence is bolstered by a secondary reaction that is even more effective. In addition, a 10,000-fold increase in the corresponding T-cell specific cytotoxic T-cells is elicited as a secondary T-cell response as a result of re-exposure to antigens.
References
- Ademokun, A. A., & Dunn-Walters, D. (2010). Immune Responses: Primary and Secondary. eLS. doi:10.1002/9780470015902.a000094
- MURRAY, I. Induction of the Primary Immune Response. Nature 217, 430–432 (1968). https://doi.org/10.1038/217430a0
- MURRAY, I. M. (1968). Induction of the Primary Immune Response. Nature, 217(5127), 430–432. doi:10.1038/217430a0
- Quast I, Tarlinton D. B cell memory: understanding COVID-19. Immunity. 2021 Feb 9;54(2):205-210. doi: 10.1016/j.immuni.2021.01.014. Epub 2021 Jan 23. PMID: 33513337; PMCID: PMC7826135.
- Zinkernagel, R. M. (2001). Regulation of the Immune Response by Antigen. Science, 293(5528), 251–253. doi:10.1126/science.1063005
- https://microbenotes.com/immune-response/#primary-immune-response
- –https://files.differencebetween.com/wp-content/uploads/2017/10/Difference-Between-T-Cell-Dependent-and-Independent-Antigen-1.pdf
- Kotsias, F., Cebrian, I., & Alloatti, A. (2019). Antigen processing and presentation. International Review of Cell and Molecular Biology. doi:10.1016/bs.ircmb.2019.07.005
- https://www.coursehero.com/file/81202410/PRIMARY-AND-SECONDARY-RESPONSEpptx/
- https://www.newhealthadvisor.org/Primary-Immune-Response.html
- https://www.merckmanuals.com/home/immune-disorders/biology-of-the-immune-system/overview-of-the-immune-system


