Table of Contents
Tumors
- Immune system tumours are classed as lymphomas or leukemias. Hodgkin’s and non-lymphomas Hodgkin’s are solid tumours that multiply in lymphoid tissues such as bone marrow, lymph nodes, and the thymus; they are also known as lymphomas.
- Leukemias are typically identified by an increase in the number of cells in the blood or lymph.
- Leukemia can arise in either the lymphoid or myeloid lineage. Historically, leukemias were classed as acute or chronic based on the disease’s clinical course.
- The acute leukemias erupted suddenly and advanced swiftly, whereas the chronic leukemias were far less aggressive and progressed slowly as mild, asymptomatic disorders.
- These clinical distinctions apply to untreated leukemias; with modern treatments, the prognosis for acute leukemias is frequently favourable, and durable remission is frequently attained.
- Now, the primary contrast between acute and chronic leukemias is the cell’s level of maturity. Chronic leukemias emerge from mature cells, whereas acute leukemias arise from immature cells.
- Acute leukemias include acute lymphocytic leukaemia (ALL) and acute myelogenous leukaemia (AML); these diseases have a quick onset and can develop at any age.
- These diseases develop slowly in adulthood and include chronic lymphocytic leukaemia (CLL) and chronic myelogenous leukaemia (CML).
- A number of B- and T-cell leukemias and lymphomas contain a translocated proto-oncogene inside the immunoglobulin or T-cell receptor genes.
- The translocation of c-myc in Burkitt’s lymphoma and mice plasmacytomas is one of the best understood.
- c-myc is translocated from chromosome 8 to the Ig heavy-chain gene cluster on chromosome 14 in 75% of Burkitt’s lymphoma patients.
- In the remaining individuals, c-myc remains on chromosome 8 and or light-chain genes are translocated to c-region myc’s 3.
- There are 9% occurrences of kappa-gene translocations from chromosome 2 to chromosome 8, and 16% occurrences of kappa-gene translocations from chromosome 22 to chromosome 8.
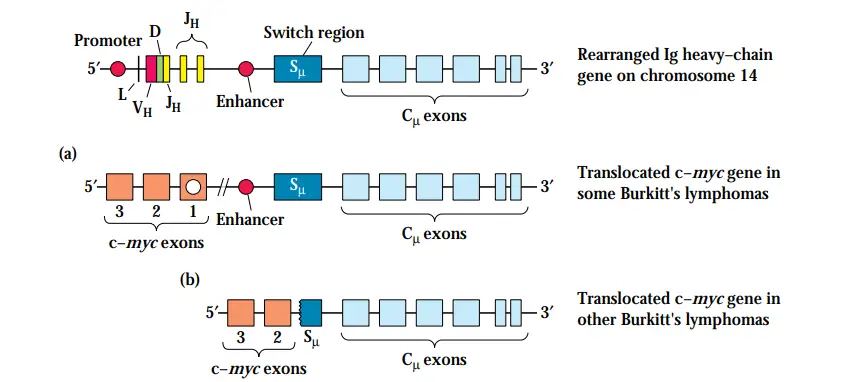
- In certain circumstances, the complete c-myc gene is translocated head-to-head to a region near the heavy-chain enhancer during translocations of c-myc to the Ig heavy-chain gene cluster on chromosome 14.
- Exons 1, 2, and 3 or exons 2 and 3 of c-myc are translocated head-to-head to the S or S switch site in other instances.
- In each instance, the translocation removes the myc coding exons from the regulatory mechanisms functioning on chromosome 8 and inserts them in the immunoglobulin-gene area, a highly active region that is constitutively produced in these cells.
- In transgenic mice, the effects of enhancer-mediated high levels of constitutive myc expression in lymphoid cells have been studied.
- In one study, mice with a transgene containing all three c-myc exons and the immunoglobulin heavy-chain enhancer were created. Within a few months of birth, thirteen of fifteen transgenic pups developed B-cell lineage lymphomas.
Tumor Antigens
- Tumor immunology is the subdiscipline that studies antigens on tumour cells and the immune response to these antigens.
- On tumour cells, both tumor-specific transplantation antigens (TSTAs) and tumor-associated transplantation antigens (TATAs) have been found (TATAs).
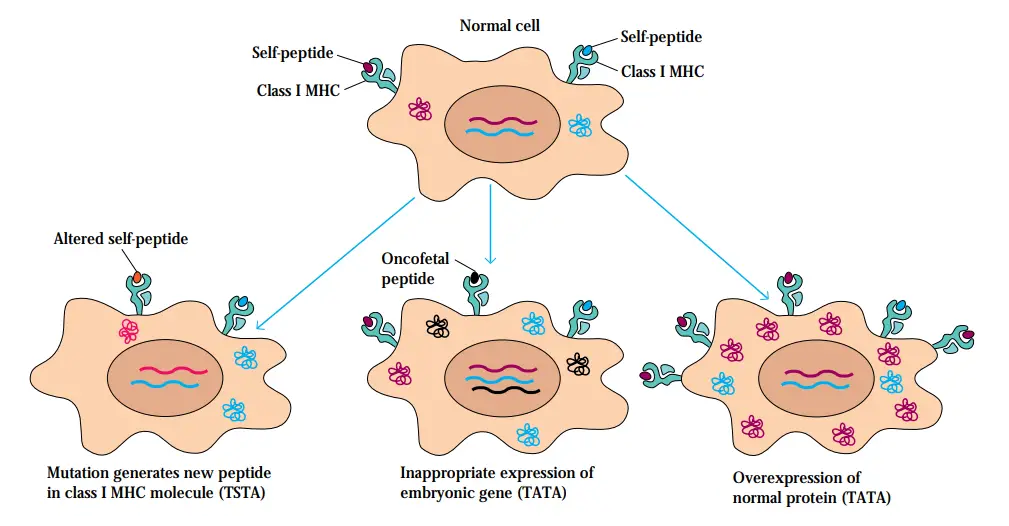
- Tumor-specific antigens are exclusive to tumour cells and are not found on normal bodily cells. Mutations in tumour cells may yield changed cellular proteins; cytosolic processing of these proteins would generate unique peptides that are presented with class I MHC molecules, eliciting a cell-mediated response from tumor-specific CTLs.
- Tumor-associated antigens, which are not exclusive to tumour cells, may be proteins expressed on normal cells during foetal development, when the immune system is immature and unable to respond, but not in adults.
- Reactivation of the embryonic genes encoding these proteins in tumour cells results in their expression in tumour cells that have undergone complete differentiation.
- Additionally, tumor-associated antigens may be proteins that are ordinarily expressed at extremely low levels on normal cells but are expressed at substantially larger levels on tumour cells.
- Currently, it is evident that the tumour antigens recognised by human T lymphocytes fall into one of four primary types.
- Antigens encoded by tumor-specifically expressed genes.
- Antigens encoded by mutant variants of normally occurring genes that have undergone mutation.
- Antigens that are generally expressed only at particular phases of differentiation or by particular lineages of development.
- Antigens that are overexpressed in specific types of cancer.
- Numerous tumour antigens are cellular proteins that give rise to peptides presented with MHC molecules; these antigens are normally identified based on their capacity to stimulate the proliferation of antigen-specific CTLs or helper T cells.
Some Antigens Are Tumor-Specific
Antigens unique to cancers caused by chemical or physical carcinogens, as well as some virally induced malignancies, have been found. It is particularly difficult to demonstrate the presence of tumor-specific antigens on spontaneously developing tumours since the immune response to such tumours destroys all of the tumour cells containing significant amounts of the antigens, hence favouring cells with low levels of the antigens.
Chemically Or Physically Induced Tumor Antigens
- Both methylcholanthrene and UV light are carcinogens that have been extensively employed to create tumour cell lines.
- When syngeneic mice are injected with deceased cells from a carcinogen-induced tumor-cell line, the animals acquire an unique immunologic response that protects them against subsequent challenge by live cells of the same line but not other tumor-cell lines.
- Even though the same chemical carcinogen induces two unique tumours at different places in the same animal, the tumour antigens are distinct, and the immune response to one tumour does not provide protection against the other tumour.
- It has been challenging to describe the tumor-specific transplantation antigens of chemically produced tumours because they cannot be detected by induced antibodies but only by their T-cell–mediated rejection.
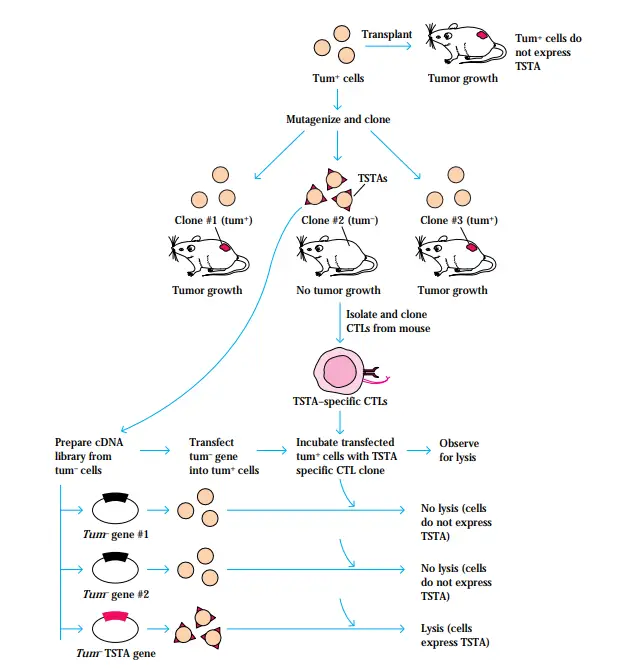
- Figure outlines one experimental method that has enabled the identification of genes encoding several TSTAs.
- When a mouse tumorigenic cell line (tum+) that produces gradually developing tumours is treated in vitro with a chemical mutagen, certain cells become incapable of forming tumours in syngeneic mice.
- These cancerous cell mutations are termed as tum– variations. It has been demonstrated that the majority of tum– variations express TSTAs that are not expressed by the original tum+ tumor-cell line.
- When tum– cells are injected into syngeneic mice, specialised CTLs detect the unique TSTAs that the tum– cells express. The TSTA-specific CTLs eliminate the tum– tumour cells, hence inhibiting tumour development.
- To identify the genes encoding the TSTAs that are expressed on a tum– cell line, the tum– cells are used to produce a cosmid DNA library. The initial tum+ cells are transfected with genes from the tum– cells.
- The expression of tum– TSTAs in transfected tum+ cells is determined by their ability to activate cloned CTLs specific for the tum– TSTA.
- Several distinct TSTAs have been identified using this method. Two techniques have facilitated the characterization of TSTAs in recent years.
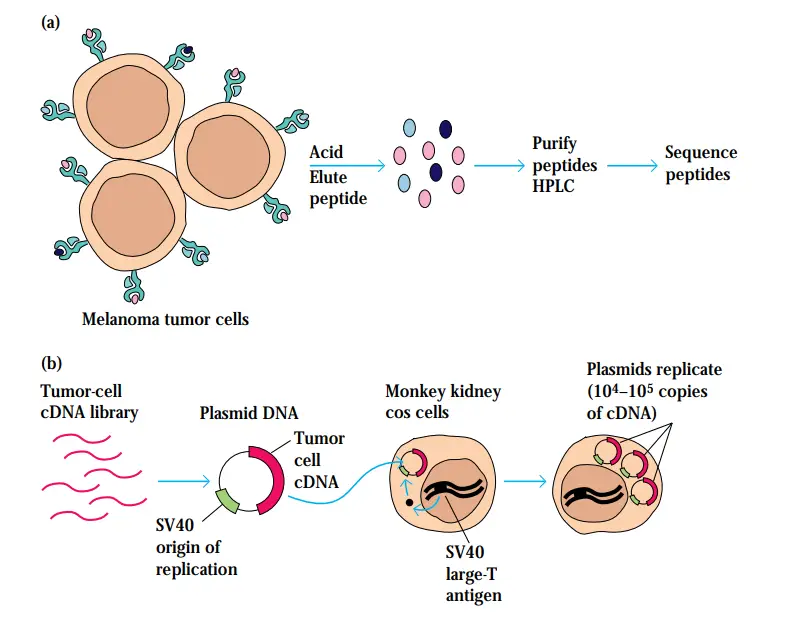
- Peptides attached to class I MHC molecules on tumour cell membranes are rinsed with acid and extracted by high-pressure liquid chromatography in one technique (HPLC).
- In some instances, sufficient peptide is eluted for Edman degradation to derive its sequence. In the second method, cDNA libraries are constructed from tumour cells.
- These cDNA libraries are transiently transfected into COS cells, which are monkey kidney cells transfected with the SV40 large-T antigen-coding gene.
- When these cells are subsequently transfected with plasmids carrying both tumor-cell cDNA and an SV40 origin of replication, the large-T antigen stimulates plasmid replication, resulting in the production of up to 104–105 plasmid copies per cell.
- This leads in large levels of tumor-cell DNA expression. It has been established that the genes encoding some TSTAs differ from normal cellular genes by a single point mutation.
- Many TSTAs are short peptides produced from cytosolic proteins that have been processed and presented in conjunction with class I MHC molecules, as suggested by further characterisation.
Viruses Induced Tumor Antigens
- In contrast to chemically produced cancers, virally induced tumours exhibit common tumour antigens.
- When syngeneic mice are injected with died cells from a specific polyoma-induced tumour, for instance, the recipients are protected against a future challenge with live cells from any polyoma-induced tumours.
- When lymphocytes from mice with a virus-generated tumour are transplanted into normal syngeneic receivers, the recipients reject all future transplantation of syngeneic cancers induced by the same virus.
- In both SV40- and polyoma-induced cancers, the presence of tumour antigens correlates with the cell’s neoplastic status. Burkitt’s lymphoma cells in humans have been shown to exhibit an Epstein-Barr virus nuclear antigen that may be a tumor-specific antigen for this kind of cancer.
- Human papillomavirus (HPV) E6 and E7 proteins are detected in over 80% of invasive cervical malignancies, making them the most prominent example of a virally encoded tumour antigen.
- As a result, there is considerable interest in evaluating as vaccine candidates the HPVs that are highly associated with cervical cancer, such as HPV-16.
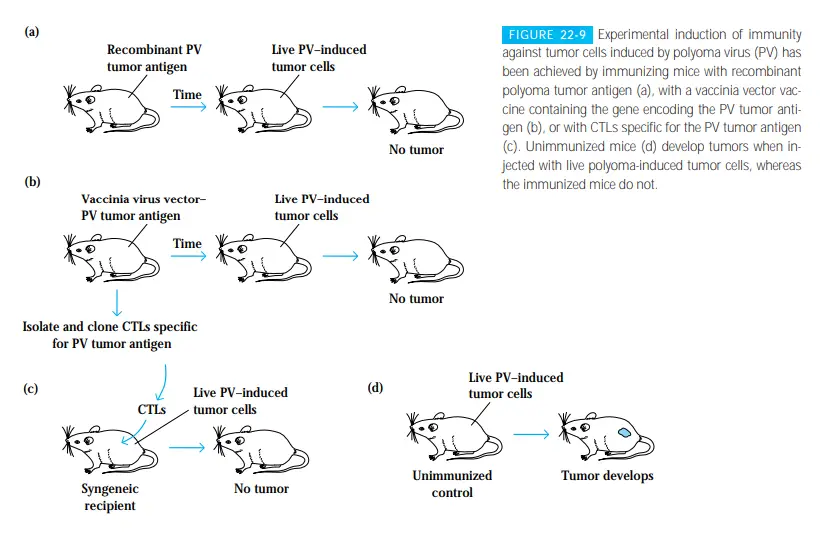
- Animal experiments demonstrate the potential utility of these virally generated tumour antigens.
- In one investigation, mice inoculated with a preparation of genetically modified polyoma virus tumour antigen were resistant to subsequent injections of polyoma-induced tumour cells.
- In another experiment, mice were inoculated with a vaccinia-virus vaccine designed with the polyoma-tumor antigen-encoding gene. In addition to developing immunity, these animals rejected subsequent injections of live polyoma-induced tumour cells.
Most Tumor Antigens Are Not Unique to Tumor Cells
- The bulk of tumour antigens are shared with normal cells and not exclusive to tumour cells.
- These tumor-associated transplantation antigens may be proteins that are typically expressed only on foetal cells and not on normal adult cells, or they may be proteins that are expressed at low levels by normal cells but at much larger levels by tumour cells.
- In this category include growth factors, growth factor receptors, and proteins encoded by oncogenes.
- On tumour cells, several growth-factor receptors are expressed at greatly elevated levels and can serve as antigens.
- Several types of tumour cells express the epidermal growth factor (EGF) receptor at 100-fold higher levels than normal cells.
- An example of an over-expressed growth factor that serves as a tumor-associated antigen is p97, a transferrin growth factor that aids in iron transport into cells.
- Melanoma cells express between 50,000 and 500,000 molecules of p97 per cell, whereas normal cells express less than 8,000 molecules per cell.
- The gene encoding p97 has been cloned, and a recombinant vaccinia virus vaccine carrying the cloned gene has been developed.
- When injected into mice, this vaccine elicited both humoral and cell-mediated immune responses, which protected the mice against live melanoma cells expressing the p97 antigen.
- These findings underscore the necessity of identifying tumour antigens as prospective therapeutic targets.
Oncofetal Tumor Antigens
- As their name suggests, oncofetal tumour antigens are found not only on malignant cells but also on normal foetal cells.
- These antigens arise early in embryonic development, before the immune system gains immunocompetence; if they later appear on cancer cells, they are recognised as foreign and elicit an immune response.
- The oncofetal antigens alpha-fetoprotein (AFP) and carcinoembryonic antigen (CEA) are the subject of extensive research (CEA). Although the serum concentration of AFP decreases from milligramme levels in foetal serum to nanogram levels in normal adult serum, the majority of liver cancer patients have increased AFP levels.
- CEA is a membrane glycoprotein present on the digestive and liver cells of foetuses between 2 and 6 months old.
- Approximately 90% of patients with advanced colorectal cancer and 50% of individuals with early colorectal cancer have elevated serum levels of CEA; some patients with other forms of cancer also have elevated serum levels of CEA.
- Due to the existence of trace quantities of AFP and CEA in some healthy adults and noncancerous illness states, the presence of these oncofetal antigens is not diagnostic of tumours, but rather aids to monitor tumour growth.
- After surgery to remove a colorectal cancer, for instance, the patient’s CEA levels are monitored. An increase in CEA level indicates resumption of tumour development.
Oncogene Proteins As Tumor Antigens
- Multiple cancers have been demonstrated to exhibit oncogene-encoded tumor-associated antigens.
- Antigens encoded by the relevant proto-oncogene are also present on normal cells.
- In many instances, there is no qualitative distinction between the oncogene and proto-oncogene products; rather, the immune system recognises the elevated levels of the oncogene product.
- As previously mentioned, human breast cancer cells show increased levels of the oncogene-encoded growthfactor receptor Neu protein, whereas normal adult cells express only trace amounts of Neu protein.
- Anti-Neu monoclonal antibodies can detect and selectively kill breast cancer cells without harming normal cells due to this differential in Neu level.
TATAS On Human Melanomas
- On human melanomas, several transplantation antigens related with tumours have been found. Five of them are oncofetal-type antigens: MAGE-1, MAGE-3, BAGE, GAGE-1, and GAGE-2.
- Each of these antigens is expressed on a substantial fraction of human melanoma tumours and a number of other human malignancies, but not on normal differentiated tissues, with the exception of the testis, where it is expressed on germ-line cells.
- In addition, melanoma cells overexpress a number of differentiation antigens expressed on normal melanocytes, including as tyrosinase, gp100, Melan-A or MART-1, and gp75, allowing them to function as tumor-associated transplantation antigens.
- a number of human melanoma tumour antigens are also present in a number of different cancers. Approximately 40% of human melanomas are MAGE-1 positive, and approximately 75% are MAGE-2 or MAGE-3 positive.
- In addition to melanomas, a substantial proportion of glioma cell lines, breast tumours, non-small-cell lung tumours, and head-and-neck carcinomas express MAGE-1, 2, or 3.
- These common tumour antigens could be utilised in the clinic. For the treatment of a number of these malignancies, it may be conceivable to develop a vaccination expressing the shared antigen.
Tumors Can Induce Potent Immune Responses
- Tumor antigens can stimulate humoral and cell-mediated immune responses in experimental animals, resulting in the elimination of tumour cells.
- In general, it appears that the cell-mediated response plays the primary function.
- Several malignancies have been found to produce CTLs that detect tumour antigens provided by class I MHC on tumour cells.
- However, as explained in the following section, the expression of class I MHC molecules is reduced in a variety of cancers, limiting the role of particular CTLs in their destruction.
Role of NK Cells and Macrophages for Tumor Recognition
- NK cell identification of malignant cells is not constrained by MHC. Thus, the decreased MHC expression of some tumour cells has no effect on the activity of these cells.
- In some instances, Fc receptors on NK cells can attach to antibody-coated tumour cells, resulting in antibody-dependent cell cytotoxicity (ADCC). The beige mutant mouse strain and the Chediak-Higashi disease in humans indicate the significance of natural killer cells in tumour immunity.
- In each instance, a genetic abnormality results in a significant impairment of NK cells and an increase in the incidence of specific forms of cancer.
- Numerous data suggest that activated macrophages play a substantial role in the immune response to malignancies. For instance, macrophages are frequently found to congregate near tumours, and their presence is frequently associated with tumour regression.
- Similar to NK cells, macrophages are not confined by MHC and have Fc receptors, allowing them to attach to antibodies on tumour cells and cause ADCC.
- Activated macrophages’ anticancer action is likely mediated by lytic enzymes and reactive oxygen and nitrogen intermediates.
- In addition, active macrophages produce the strong antitumor cytokine tumour necrosis factor (TNF-alpha). It has been discovered that injecting TNF-alpha into animals with tumours induces tumour bleeding and necrosis.
Immune Surveillance Theory
- Paul Ehrlich first conceived of the principle of immunological surveillance in the early 20th century. He claimed that cancer cells frequently develop in the body, but are identified as alien and destroyed by the immune system.
- Approximately fifty years later, Lewis Thomas proposed that the immune system’s cell-mediated branch had evolved to patrol the body and remove cancer cells.
- Tumors can only develop if cancer cells are able to evade immune monitoring, either by decreasing their expression of tumour antigens or by a reduction in the immune response to these cells.
- The higher frequency of cancer in transplant patients on immunosuppressive drugs was one of the early observations that appeared to corroborate the immune surveillance theory. However, it was challenging to reconcile other data with this notion.
- For instance, nudized mice lack a thymus and, consequently, functioning T lymphocytes. According to the notion of immune surveillance, these mice should have a higher incidence of cancer; yet, they are no more susceptible to cancer than other mice.
- Contrary to what the theory predicts, the incidence of other frequent cancers (such as lung, breast, and colon cancer) is not increased in patients taking immunosuppressive medicines, even though there is an increased incidence of tumours of the immune system.
- The immunosuppressive medicines themselves may have a direct carcinogenic effect on immune cells, which could account for the selective increase in malignancies of the immune system.
- The immune surveillance idea is also incongruous with the experimental findings concerning the effect of tumor-cell quantity on the immune system’s ability to respond.
- Animals injected with either low or extremely high concentrations of tumour cells grow tumours, whereas animals injected with intermediate amounts do not.
- It is difficult to reconcile the method through which a small number of tumour cells “slip past” with the hypothesis of immune surveillance.
- Lastly, this idea assumes that there are qualitative antigen distinctions between cancer cells and normal cells.
- As stated previously, many forms of cancers do not express tumor-specific antigens, and any immune response must be induced by quantitative variations in antigen expression between normal cells and tumour cells.
- Nevertheless, malignancies generated by viruses should exhibit antigens encoded by the viral genome.
- These antigens are fundamentally distinct from those expressed by normal tissues and should draw the immune system’s attention. There are numerous examples of unique immune responses to malignancies caused by viruses.
- Nevertheless, with the exception of tumours caused by viruses, it is currently unproven that malignant tumours occur exclusively when the immune system is in some way compromised or when tumour cells lose their immunogenicity, allowing them to evade immune monitoring.
- Despite this, it is evident that an immune response can be created in response to tumour cells, and therapeutic strategies aiming at enhancing this response may act as a defence against malignant cells.
Tumor Evasion of the Immune System
Although it is evident that the immune system may respond to tumour cells, the fact that so many people die annually from cancer implies that this response is frequently unsuccessful. This section discusses different strategies by which tumour cells elude the immune system.
Anti-Tumor Antibodies Can Enhance Tumor Growth
- Following the finding that antibodies to tumor-specific antigens could be created, attempts were undertaken to protect animals from tumour growth via active immunisation with tumour antigens or passive immunisation with antitumor antibodies.
- To the researchers’ great surprise, these vaccines did not protect against tumour growth; in fact, they frequently promoted tumour growth.
- Subsequently, cell-mediated lympholysis (CML) reactions were used to examine the tumor-promoting potential of immunological sera.
- Serum extracted from animals with advancing tumour growth was observed to inhibit the CML reaction, whereas serum extracted from animals with regressing tumours had little or no blocking efficacy. K. E. and I. Hellstrom extended these findings by demonstrating that children with progressive neuroblastoma had elevated levels of a blocking factor in their sera, whereas children with regressive neuroblastoma did not.
- Since these first reports, a number of human cancers have been linked to blocking factors.
- In certain instances, the anticancer antibody itself functions as a blocking agent. The antibody presumably attaches to tumor-specific antigens and conceals them from cytotoxic T cells. In many instances, the blocking factors are antibodies complexed with tumour antigens rather than antibodies alone.
- Although it has been demonstrated that these immunological complexes limit the CTL response, the mechanism behind this inhibition is unknown.
- Complexes may also hinder ADCC by binding to Fc receptors on NK cells or macrophages and inhibiting their function.
Antibodies Can Modulate Tumor Antigens
- Certain tumor-specific antigens have been reported to vanish from the surface of tumour cells in the presence of serum antibody before reappearing when the antibody is absent.
- When leukemic T cells are injected into mice that have previously been inoculated with a leukemic T-cell antigen, this effect, known as antigenic modulation, is clearly detected (TL antigen).
- These mice produce large concentrations of anti-TL antibody, which binds to the TL antigen on leukemic cells and promotes capping, endocytosis, and/or shedding of the antigen-antibody complex.
- As long as the antibody is present, these leukemic T cells will not express the TL antigen and so cannot be eradicated.
Tumor Cells Frequently Express Low Levels of Class I MHC Molecules
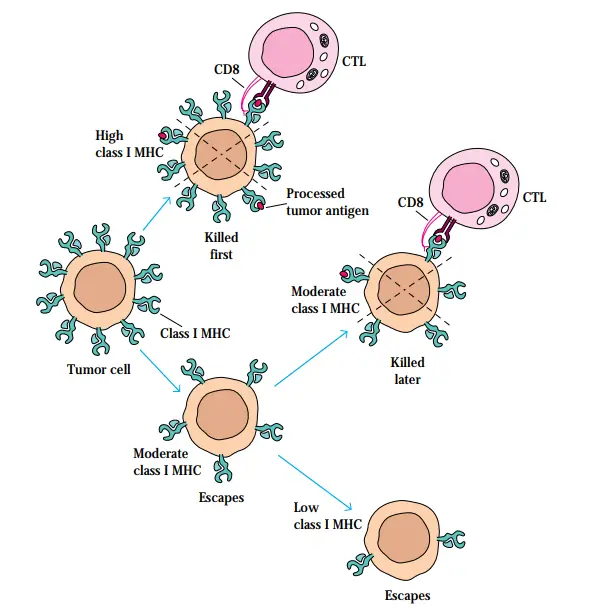
- Since CD8+ CTLs detect only antigen linked with class I MHC molecules, any change in the expression of class I MHC molecules on tumour cells may have a significant impact on the CTL-mediated immune response.
- Several malignancies have been found to have lower numbers of class I MHC molecules, which is commonly associated with malignant transformation of cells.
- The absence of MHC molecules on a tumour is often indicative of a negative prognosis, given that a decrease in class I MHC expression is often associated by increased tumour growth.
- The immune response itself may play a role in choosing tumour cells with reduced expression of class I MHC.
Tumor Cells May Provide Poor Co-Stimulatory Signals
- T-cell activation requires an activating signal, which is initiated by the T-cell receptor’s detection of a peptide–MHC complex, and a co-stimulatory signal, which is caused by the interaction of B7 on antigen-presenting cells with CD28 on T cells.
- Both signals are necessary to stimulate IL-2 synthesis and T cell proliferation. Lack of co-stimulatory molecules may contribute significantly to the poor immunogenicity of many tumour cells.
- In the absence of sufficient numbers of antigen-presenting cells in close proximity to a tumour, T cells will only get a partial activation signal, which may result in clonal anergy.


