Table of Contents
What is Osmoregulation?
- Osmoregulation is a critical biological process that involves the maintenance of constant osmotic pressure in the fluids of an organism, which is essential for the stability of the organism’s internal environment. This process is fundamental for the survival of all living organisms as it ensures the optimal functioning of cells by controlling the balance of water and electrolytes in their bodies.
- The mechanism of osmoregulation begins with the detection of water and solute levels by osmoreceptors. These specialized sensors are adept at monitoring the osmotic pressure, which is a measure of the force with which water moves across a semipermeable membrane due to osmosis. Osmosis, in this context, refers to the movement of water from a region of lower solute concentration to one of higher solute concentration.
- In environments where the osmotic pressure is variable, organisms must exert a regulatory force to maintain equilibrium. This is particularly evident when considering a hypertonic solution, where the solute concentration is higher outside the cell than inside. To prevent the inward rush of water, which could lead to cell swelling and potential damage, the organism must adjust its internal pressure accordingly.
- The regulation of osmotic pressure is not a static process but one that adjusts to the organism’s changing needs. Despite fluctuations that may occur on an hourly or daily basis, an organism typically achieves an osmotic steady state over the long term. This dynamic equilibrium is crucial for both aquatic and terrestrial organisms, which face different challenges in their respective environments.
- To maintain osmotic balance, organisms employ various excretory mechanisms. These include the removal of metabolic nitrogen wastes, which are byproducts of protein metabolism, and other potentially harmful substances like excess hormones. The excretory system, which encompasses organs such as the skin and kidneys, plays a pivotal role in this process. The kidneys, for instance, are instrumental in filtering the blood, reabsorbing necessary substances, and excreting waste in the form of urine.
- Therefore, osmoregulation is not merely a passive occurrence but a complex and active physiological process. It involves a series of responses and adjustments that are vital for the organism’s survival, growth, and overall health. The ability to maintain osmotic balance enables organisms to thrive in a diverse array of habitats, from the arid deserts to the depths of the oceans.
Role of ADH, Renin-Angiotensin and Aldosterone in Osmoregulation
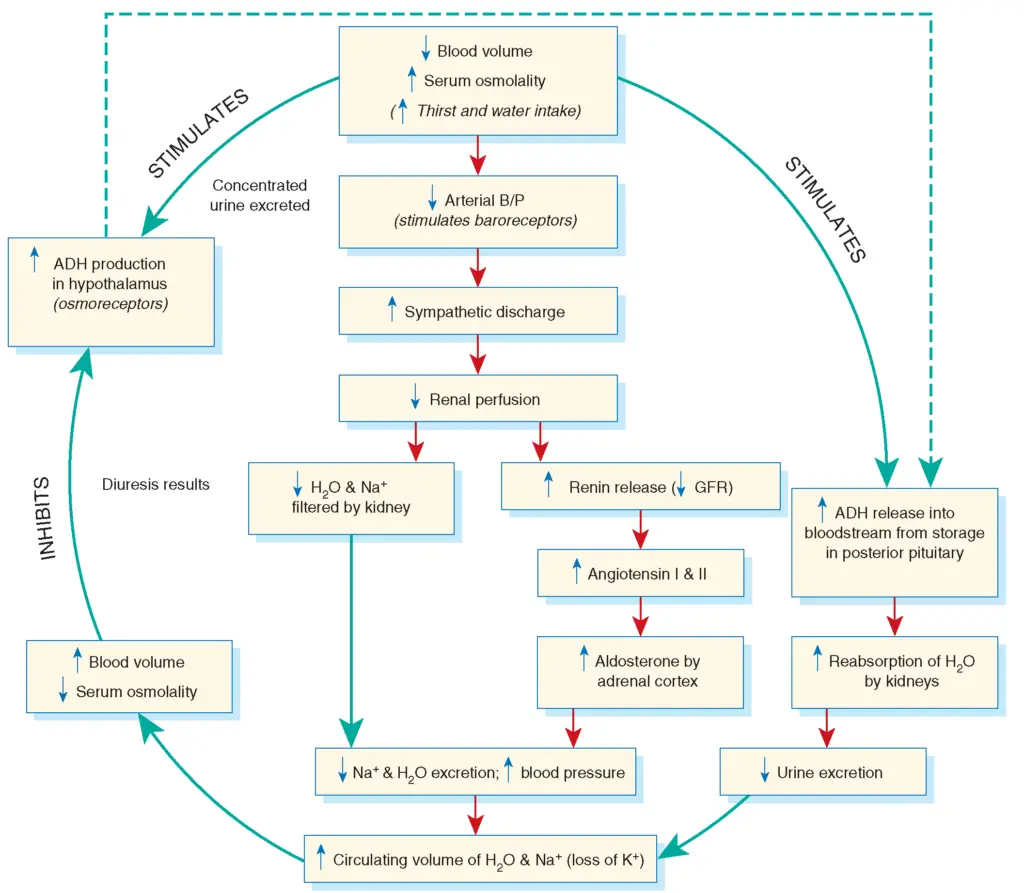
1. Role of ADH (Anti-diuretic Hormone) in Osmoregulation
The role of the antidiuretic hormone (ADH), also known as vasopressin, in osmoregulation is pivotal for maintaining the body’s water balance and ensuring the stability of its internal environment. Here’s a detailed and sequential explanation of ADH’s role in osmoregulation:
- Synthesis and Secretion: ADH is synthesized in the neurons of the hypothalamus. After synthesis, it is transported to the posterior pituitary gland, where it is stored and later secreted into the bloodstream.
- Detection of Osmotic Pressure: The hypothalamus contains osmoreceptors that are sensitive to changes in the osmotic pressure of the blood. When these osmoreceptors detect an increase in the osmotic pressure, indicating that the blood is becoming more concentrated (due to dehydration, for instance), they signal the posterior pituitary gland to release ADH.
- Action on the Kidneys: Once released, ADH travels to the kidneys, where it acts on the cells of the distal convoluted tubules and collecting ducts. Specifically, it increases the permeability of these tubules and ducts to water by promoting the insertion of water channels, known as aquaporins, into their cell membranes.
- Water Reabsorption: Due to the action of ADH, more water is reabsorbed from the filtrate in the kidneys back into the bloodstream. This process reduces the volume of urine produced and increases its concentration, ensuring that the body retains more water.
- Restoration of Blood Osmolarity: As more water is reabsorbed into the bloodstream, the osmolarity of the blood decreases, moving it closer to its ideal concentration. This helps in maintaining the body’s internal fluid balance.
- Negative Feedback Mechanism: As the osmolarity of the blood returns to its set point, the osmoreceptors in the hypothalamus detect this change and reduce the signal for ADH secretion. This negative feedback mechanism ensures that the right amount of ADH is secreted to maintain the body’s water balance.
- Situations of Low Osmolarity: If the osmoreceptors detect a decrease in blood osmolarity (indicating an excess of water in the blood), the secretion of ADH is reduced. This results in decreased water reabsorption in the kidneys, leading to the production of a larger volume of dilute urine, helping the body get rid of the excess water.
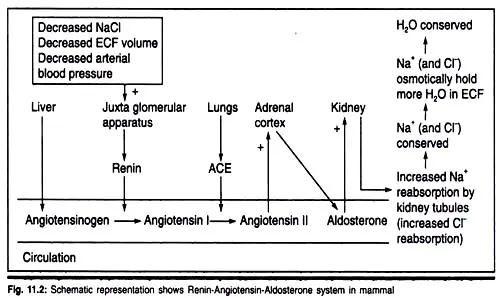
2. Role of Renin-Angiotensin system in Osmoregulation
The Renin-Angiotensin system (RAAS) is a sophisticated regulatory mechanism that plays a vital role in osmoregulation, ensuring the maintenance of blood pressure and fluid balance within the body. Here’s a detailed and sequential explanation of its role:
- Detection of Sodium Levels: When there’s a decrease in the sodium (Na+) level in the blood, it leads to a subsequent decrease in both blood volume and interstitial fluid level. This is because a reduced sodium concentration means less water enters the blood by osmosis. Consequently, blood pressure drops, signaling the need for the RAAS to be activated.
- Activation of Juxtaglomerular Apparatus: The drop in blood pressure is detected by a specialized group of sensory cells located in the juxtaglomerular apparatus. This apparatus is situated at the point where the distal convoluted tubule (DCT) intersects with the afferent and efferent arterioles of the renal system.
- Release of Renin: In response to the detected decrease in blood pressure, the cells of the juxtaglomerular apparatus secrete the enzyme renin. This enzyme plays a pivotal role in the next step of the RAAS.
- Conversion to Angiotensin I: Renin acts on a substrate called angiotensinogen, which is present in the blood, converting it into angiotensin I.
- Formation of Angiotensin-II: Angiotensin I, which is relatively inactive, is then converted into the potent peptide hormone, angiotensin-II. This conversion is facilitated by the angiotensin-converting enzyme (ACE).
- Functions of Angiotensin-II: Angiotensin-II has multiple effects that aim to restore blood pressure and osmotic balance:
- Sodium Reabsorption: Angiotensin-II stimulates the proximal convoluted tubules in the kidneys to reabsorb sodium. By retaining sodium, the osmotic pressure of the blood increases. This, in turn, reduces the loss of water from the renal tubules, ensuring that more water is reabsorbed back into the bloodstream.
- Vasoconstriction: Besides its role in sodium reabsorption, angiotensin-II also directly raises blood pressure by causing the constriction of blood vessels. This vasoconstriction results in increased resistance, thereby elevating blood pressure.
2. Role of Aldosterone hormone in Osmoregulation
Aldosterone, a steroid hormone, plays a pivotal role in osmoregulation, ensuring the body maintains a balanced internal environment. Its primary function revolves around the regulation of sodium and potassium ions in the body, which in turn affects fluid balance and blood pressure. Here’s a detailed and sequential explanation of aldosterone’s role in osmoregulation:
- Origin and Secretion: Aldosterone is produced and secreted by the adrenal cortex, specifically the zona glomerulosa, which is the outermost layer of the adrenal glands located atop each kidney.
- Stimulus for Release: The primary stimulus for aldosterone secretion is the activation of the Renin-Angiotensin system (RAAS). When blood pressure drops or when there’s a decrease in blood sodium levels, the RAAS is activated, leading to the production of angiotensin II. Angiotensin II, in turn, stimulates the adrenal cortex to release aldosterone.
- Action on the Kidneys: Once released, aldosterone acts on the cells of the distal convoluted tubules and collecting ducts in the kidneys. Its primary action is to promote the reabsorption of sodium ions (Na+) and the excretion of potassium ions (K+).
- Sodium and Water Balance: By promoting sodium reabsorption, aldosterone ensures that the body retains sodium. As sodium is reabsorbed, water follows osmotically, leading to an increase in blood volume and, consequently, an increase in blood pressure.
- Potassium Regulation: Besides its role in sodium regulation, aldosterone also ensures that potassium levels in the body are kept in check. By promoting the excretion of potassium into the urine, aldosterone helps maintain the body’s potassium balance.
- Feedback Mechanism: The body employs a negative feedback mechanism to regulate aldosterone secretion. As blood pressure rises and sodium levels are restored, the stimulus for aldosterone release diminishes, ensuring that the hormone’s levels in the bloodstream are kept within a narrow range.
- Interaction with Other Systems: Aldosterone’s actions are closely linked with other systems, especially the RAAS. Besides angiotensin II, other factors like elevated potassium levels in the blood can also stimulate aldosterone release.


