Table of Contents
What are Poxviruses?
- Poxviruses are the largest and most complicated viruses found in people, animals, birds, and insects.
- These viruses, which belong to the family Poxviridae, are a broad group of morphologically identical DNA viruses that share a nucleocapsid protein.
- Poxviruses are the largest and most complicated viruses that infect vertebrates; they are large enough to be observed under a light microscope.
- The eradication of smallpox is the greatest success story in the fight against infectious disease, and it offers numerous significant lessons.
- This epic contains at least three “firsts”: the first vaccine, the first disease eradicated entirely by immunisation, and the first virus infection against which treatment was clinically effective.
Classification of Poxviruses
Based on whether they infect insect or vertebrate hosts, the family Poxviridae has been divided into two subfamilies: Chordopoxvirinae and Entomopoxvirinae. The subfamily Chordopoxvirinae encompasses viruses that infect vertebrate hosts and consists of eight genera, at least four of which cause human illness. These are the categories:
- Orthopoxvirus: The genus Orthopoxvirus contains the mammalian poxviruses, including smallpox (variola), vaccinia, monkeypox, cowpox, buffalopox, rabbitpox, mousepox, and camelpox.
- Parapoxviruses: Parapoxviruses are viruses of ungulates that can occasionally cause illnesses in humans. These viruses are orf viruses, pseudocowpox virus, deerpox viruses, and bovine papular stomatitis virus.
- Yatapoxviruses: Yatapoxviruses include tanapox and yabapox viruses, which are primarily found in Africa. These viruses include the molluscum contagiosum virus.
The genera Orthopoxvirus and Parapoxvirus contain the majority of poxviruses that cause illness in humans. The virus that causes smallpox and the virus that causes molluscum contagiosum are particular human pathogens, but other poxviruses cause rare zoonotic illnesses in humans.
Morphology of Poxviruses
- These are the largest viruses ever discovered.
- The orthopoxviruses have a brick-like form.
- They measure approximately 230 270 nm and, when appropriately stained, can be observed with a standard light microscope.
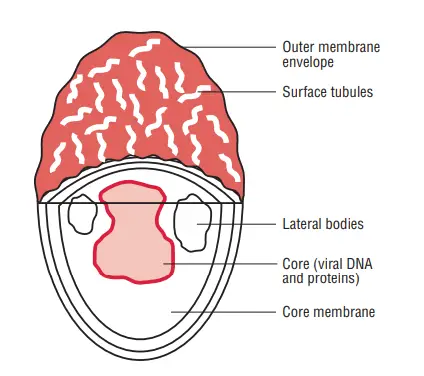
- The poxviruses have a complicated structure that is neither icosahedral nor helical. The virion contains a dumbbell-shaped core structure and two lateral bodies, named for their position within the virion.
- In 1887, Buist first observed the Variola virus under a microscope.
- In 1906, Paschen created a staining method for viral particles and demonstrated the elementary bodies (Paschen bodies) in smallpox lesion smears.
Physical and Chemical Properties
- Poxviruses are stable and, if shielded from sunlight, can remain alive at room temperature for months.
- They can persist for years when frozen or freeze-dried.
- They are sensitive to UV light and other types of radiation.
- They are resistant to 50% glycerol and 1% phenol, but are easily rendered inactive by formalin and oxidising disinfectants.
Antigenic Structure
- All poxviruses possess a nucleoprotein (NP) antigen in common.
- Approximately twenty distinct antigens have been found using immunodiffusion.
- These antigens include the LS antigens (a compound of two antigens, the heat labile L and the heat stable S antigens), agglutinogen, and hemagglutinin, which is responsible for the nonspecific agglutination of erythrocytes by tissue lipids.
Cultivation and Host Range
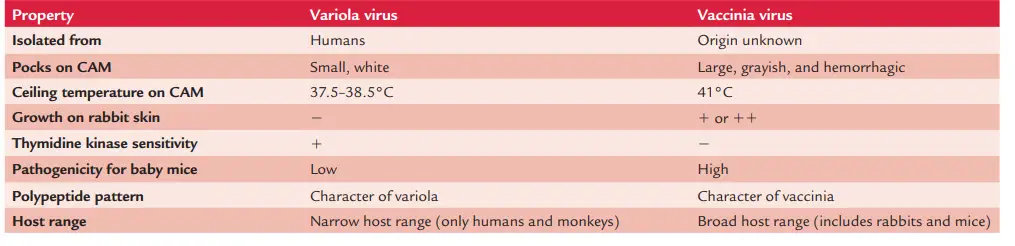
The variola and vaccinia viruses can be differentiated by their growth characteristics and host range.
Chick Embryo
- By inoculating vesicular fluid onto the chorioallantoic membrane (CAM) of chick embryos, viruses are isolated.
- Both vaccinia and variola viruses produce pocks in 48-72 hours on the CAM of 11- to 13-day-old chick embryos.
- Variola papules are small, lustrous, white, convex, non-necrotic, non-hemorrhagic, non-necrotic lesions.
- Vaccinia papules are bigger, irregular, flat, grey, necrotic, and sometimes hemorrhagic lesions.
Tissue Culture
- Viruses such as variola and vaccinia can be cultivated in tissue cultures of monkey kidney, HeLa, and chicken embryo cells.
- Vaccinia produces cytopathogenic effects within 24 to 48 hours, but variola takes longer.
- In stained preparations, eosinophilic inclusion bodies—Guarnieri bodies—can be observed.
- The inclusion bodies are composed of viral particle aggregates in a matrix. Vaccinia virus creates plaques in chick embryo tissue cultures but not variola virus.
Animals
- Scarification can infect monkeys, calves, lambs, and rabbits, leading to vesicular lesions.
Variola and Vaccinia Viruses
Variola Viruses
- The virus variola is responsible for causing smallpox.
- Variola has a limited spectrum of hosts (only humans and monkeys).
- Historically, there were two separate clinical forms of smallpox.
- Variola major or classical smallpox: Variola major, or classical smallpox, is a highly deadly, virulent disease prevalent in Asia.
- Variola minor or alastrim: Variola minor, often known as alastrim, is a mild, nonfatal condition mainly found in Latin America.
- Variola major and minor were antigenically identical, but their biological properties were distinct.
- They were stable variations, as the sickness generated by each consistently produced genuine offspring. Smallpox was not transmitted by Alastrim, and vice versa.
Vaccinia Virus
- Vaccinia virus, the pathogen used for immunisation against smallpox, is a unique species of Orthopoxvirus.
- Vaccinia virus is exceptional in that it is a “artificial virus” that does not arise in nature.
- It may be the result of genetic recombination, a new species formed from cowpox or variola virus by serial transfer, or a descendent of a now-extinct viral genus.
- Vaccinia has a vast host range, which includes rabbits and mice, whereas variola has a limited host range.
- Vaccinia virus is safer to work with than variola, hence it has been examined in greater depth.
- As a vector for the generation of recombinant vaccines, vaccinia virus is utilised.
- The genome of vaccinia can accommodate approximately 25,000 foreign base pairs, adequate for the introduction of several genes.
- Numerous genes have been introduced, including those coding for hepatitis B viral antigens, HIV antigens, rabies antigens, and pharmacologically significant neuropeptides.
Control of Smallpox
- Edward Jenner discovered in 1796 that vaccination with cowpox could prevent smallpox.
- Jenner deserves credit for demonstrating that following the inoculation of young James Phipps with cowpox virus on May 14, 1796, purposeful inoculation with smallpox material did not elicit the disease.
- Smallpox has been a plague for thousands of years, bringing death and disfigurement.
- The global eradication of smallpox, accomplished after ten years of concentrated campaigns under the aegis of the WHO, represents one of the most remarkable medical achievements in history.
- The eradication of naturally occurring smallpox occurred in 1977.
- The WHO declared the global eradication of smallpox on May 8, 1980.
Other Poxvirus Diseases
Vaccines
- The vaccination against smallpox is a live preparation of vaccinia virus grown on the skin of cows.
- The vaccine is administered via scarification, which results in a local pustule that heals with the creation of a scab.
- The virus is then cultured on the skin of calves to limit the chance of syphilis and other infections being transmitted during vaccination.
- Edward Jenner initially infected with pustules harbouring the cowpox virus.
- Vaccinia virus used as a vaccine replicates at the injection site, resulting in the formation of erythematous maculopapules.
- Over the course of 10–14 days, these lesions vesiculate and finally cure by generating a scab.
- The lesions are resolved by the production of pustules, which are then followed by scaling and healing.
- The remission of the condition is connected with the establishment of a 10-year-long immunity to variola infection.
Vaccinia Virus
- Vaccinia virus is unique in that it was created in a laboratory and does not occur in nature.
- Vaccinia virus was employed as a vaccination against smallpox.
- Edward Jenner initially employed the cowpox virus for smallpox immunisation.
- In later years, the original viral strain was kept alive through arm-to-arm inoculation and by preserving dried material on threads.
- Over time, the strain of vaccinia currently used in vaccinations inexplicably underwent several lasting alterations from its original cowpox form.
- This vaccinia virus could be distinguished from fresh isolates of cowpox and smallpox viruses with relative ease.
- Vaccinia is currently being examined in greater depth than variola since it is safer to work with.
- Additionally, the virus is employed as a vector for the generation of recombinant vaccines. Vaccinia and variola viruses share a morphological similarity.
- However, they can be distinguished by their growth characteristics and host range.
- Recent evidence indicates that Vaccinia virus is closely linked to the New World orthopoxviruses Cantagalo and Aracatuba.
- Vaccinia virus can be in vitro cultivated on CAM.
- On the CAM, the virus is identifiable by a distinctive pock lesion.
- The vaccinia virus causes significantly larger, irregular, flat, necrotic, and often hemorrhagic lesions.
- Vaccinia virus, which is utilised for immunisation, can also infect humans. Vaccinia induces infection through unintentional skin inoculation.
- The lesion begins as a maculopapular rash at the site of infection, then progresses to vesicles, pustules, and finally scab formation.
- The lesion heals with the production of a noticeable scar.
- Vaccinia virus produces eczema vaccinata in patients with dermatitis and progressive vaccinia in persons with immunodeficiency.
Monkeypox
- The monkeypox virus can infect people and result in an illness comparable to smallpox.
- This virus was first isolated in 1958 in Copenhagen from caged monkeys.
- In the early 1970s, the first human infection with this virus was documented.
- In West and Central Africa, particularly in Zaire, cases of monkeypox have been documented as a rare zoonotic illness.
- In 2003, further instances of monkeypox were detected in North America.
- The origin of the virus was identified to Africa-imported exotic rats.
- The transmission of monkeypox occurs through contact with diseased animals, such as monkeys and squirrels.
- Transmission from person to person is uncommon.
- Clinically, monkeypox and smallpox are indistinguishable.
- The condition is characterised by the appearance of a widespread pustule, rash, fever, and toxaemia.
- Electron microscopy is effective for diagnosing a disorder by demonstrating virion particles in clinical specimens.
Buffalopox
- In India, buffaloes contract buffalopox, which is believed to be caused by the vaccinia virus.
- Viruses cause pustular sores on the teats and udders of breastfeeding buffaloes that are infected.
- Those who come into contact with these diseased buffaloes, such as milkmen, contract the virus.
- Typically, sores appear on the hands and faces of milkmen.
- The virus that causes buffalopox appears to be different from variola and vaccinia. The vaccination against smallpox does not protect against infection with buffalopox.
Cowpox
- Cowpox infection in humans is typically an occupational danger.
- Cowpox is similar to variola and vaccinia viruses antigenically, but may be distinguished by the hemorrhagic lesions it causes on CAM and rabbit skin.
- Cows infected with cowpox develop lesions on their teats and udders. During the process of milking, it may spread to other cows and humans.
- Natural cowpox infection has also been observed in zoo-kept wild animals, such as cheetahs and elephants, as well as domestic cats.
- It has been suggested that rodents or cats, and not cows, are the major hosts of cowpox infection.
- Milker’s node, also known as paravaccinia, is an occupational disease that individuals develop while milking sick cows.
- Common lesions include tiny nodules with ulceration.
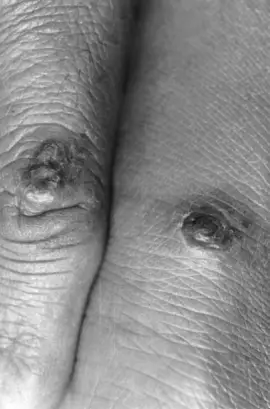
- The illness manifests as painful, bleeding sores on the hands and face (Color Image 55) accompanied by fever and other constitutional abnormalities.
- Unlike cowpox, the virus develops in bovine kidney cell culture but not in embryonated eggs.
Orf
- Orf is a human infection caused by the infectious pustular dermatitis virus of sheep and goats.
- The disease manifests as a single persistent granulomatous lesion with a central ulcer in people.
- Lesions typically appear on the hands, forearms, and infrequently the face. The wounds heal without leaving scars.
- Morphologically, the virus resembles paravaccinia virus.
Molluscum Contagiosum
- Molluscum contagiosum is a poxvirus peculiar to humans.
- The virus is transmitted through close touch, typically sexual contact.
- The virus causes a skin illness that typically affects children and young adults.
- It generates tiny, pink, pearl-like papular neoplasms of the skin or mucous membranes.
- These lesions exist on the epidermis and are seen on the majority of body parts, excluding the soles and palms.
- Lesions are most prevalent in the trunk and anogenital regions.
- This is a self-limiting condition, which often resolves itself over time.
- Molluscum contagiosum can cause chronic and severe skin sores in HIV-positive people.
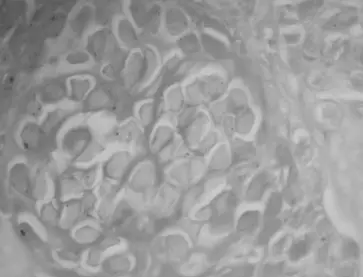
- Molluscum bodies are hyaline acidophilic inclusion structures observed in sections of nodular lesions.
- Their bodies are made of many virion particles encased in a protein matrix and measure 20–30 m in length.
- These inclusion bodies are visible in the stratum corneum and stratum granulosum cells.
- Only humans are susceptible to infection. The virus cannot be grown in animals, embryonated eggs, or tissue cultures.
Tanapox
- In the 1950s, the Tanapox virus was initially discovered from episodes of febrile sickness along the Tana river in Kenya.
- The virus causes solitary, vesicular lesions on the skin, which typically do not develop into pustules.
- This lesion is most frequently observed on the upper body.
- The virus is transmitted by insect bites from monkeys and other reservoirs of wild animals. It has no antigenic relationship with other poxviruses.
- The virus replicates in human and monkey tissue cultures, but not in embryonated eggs.
Yabapox
- Monkeys with Yabapox virus develop huge benign tumours.
- It causes benign histiocytomas in monkeys 5–20 days following subcutaneous or muscle inoculation.
- Such lesions have been recorded among individuals who have handled infected monkeys.
Variola (Smallpox) Virus
Following an extensive worldwide campaign by the World Health Organization, the variola virus-caused disease smallpox was eradicated from the planet in 1980. (WHO). However, the potential use of the smallpox virus as a bioterrorism agent is currently the primary concern.
Morphology of Variola (Smallpox) Virus
- The variola virus is a big, brick-shaped virus that measures 300 200 200 nm and is nearly visible under a light microscope.
- The virion is composed of 90% protein, 5% lipid, and 3% DNA.
- The viral genome is composed of a big, double-stranded, linear DNA with both ends joined. The DNA ranges in size from 130 to 375 kbp and features a terminal loop.
- The external virion has two envelopes, whereas the intracellular virion has only one. The outer envelope surrounding the extracellular virion is composed of lipids from the host cell and various virus-specific proteins, including hemagglutinins. These virions include a significant number of proteins (more than 100), at least ten of which exhibit the enzymatic activity necessary for genome replication.
- Multiple enzymes on the virus aid in the production, polyadenylation, and methylation of viral messenger RNA (mRNA).
Viral replication of Variola (Smallpox) Virus
- Replication of poxviruses is complex. They are uncommon among DNA viruses in that their whole replication cycle occurs in the cytoplasm of the host cell.
- The virus encodes the enzymes necessary for the creation of mRNA and DNA, which are crucial for genetic replication.
- The virus encodes and transports all proteins required for mRNA production.
- Additionally, the virus encodes proteins for tasks such as DNA synthesis and immune evasion.
- As they are liberated from the cell, the virions acquire their envelopes by budding from the cell membrane.
Susceptibility to physical and chemical reagents
- The most stable conditions for the Variola virus are low temperature and low humidity.
- It is viable for months at room temperature if shielded from sunlight and kept in the cold, or for years when freeze-dried.
- It is impervious to the effects of 50% glycerol and 1% phenol.
- Even though the virus is enclosed, it is not vulnerable to ether and is hence not inactivated by ether.
- It is vulnerable to ultraviolet light and other irradiations, as well as formalin and other oxidising disinfectants.
Antigenic properties
- The smallpox virus has a single serotype, which was responsible for the disease’s successful vaccine.
- All poxviruses, including vaccinia viruses, possess a nuclear protein antigen that is shared by all.
- At least 20 distinct antigens, including LS antigen, agglutinogen, and hemagglutinin, are present on these poxviruses.
Poxviruses Isolation and Animal Susceptibility of of Variola (Smallpox) Virus
Chick embryo
- In chick embryos, both variola and vaccinia viruses proliferate.
- Within 48–72 hours, they generate pocks on the chorioallantoic membrane (CAM) of 11–13-day-old chick embryos.
- Small, shiny, white, convex, non-necrotic, and non-hemorrhagic papules are produced by the Variola virus.
- Vaccinia viruses cause bigger, irregular, grey, necrotic, and sometimes hemorrhagic papule lesions.
Cell culture
- The virus may be cultured in cells derived from chick embryos, monkey kidneys, and HeLa cells.
- In contrast to the vaccinia virus, which generates cytopathic effects (CPEs) within 24–48 hours, the variola virus generates CPEs relatively slowly.
- The CPEs are composed of Guarnieri bodies, which are eosinophilic inclusion bodies composed of virus particle aggregation in matrix.
- These can be illustrated using stained specimens.
Laboratory animals
- Only monkeys are experimentally infected with the variola virus.
- The variola virus produces smallpox in monkeys with generalised skin lesions following intranasal infection.
- Scarification of rabbit cornea with variola virus results in keratitis with the presence of distinctive Guarnieri bodies in stained corneal smears.
Pathogenesis and Immunity of Variola (Smallpox) Virus
Pathogenesis of small pox
- The variola virus causes smallpox, which is transmitted through inhalation of nasal, oral, or pharyngeal droplets.
- Additionally, the infection can be contracted through direct contact with contaminated skin or fomites. The virus enters the human host through the upper respiratory mucous membranes.
- Poxviruses encode a large number of proteins that initially drive host cell growth and ultimately lead to cell lysis and viral spread, aiding their replication in infected cells, cell lysis, and viral spread.
- The virus replicates at the injection site and travels to lymph nodes draining the mucosal entrance site.
- The virus replicates in lymphoid organs, triggers transitory viremia, and infects reticuloendothelial cells.
- This is then followed by a secondary phase of growth in these cells, which results in a secondary viremia.
- This results in the disease’s clinical signs, which include fever and other toxic indications.
- The virus then enters the skin, localises in the skin’s blood vessels, and causes the characteristic rash of smallpox.
- The rash is induced by the multiplication of viral in the skin, followed by the destruction of virus-infected cells by cytotoxic T cells.
Host immunity
- Infection with Variola is marked by the development of both humoral and cellular immunity.
- Within the first to third week of infection, hemagglutination inhibition (HI), complement fixing (CF), and neutralising (NT) antibodies emerge as part of the humoral immune response.
- The levels of HI and CF antibodies typically decline within a year, whereas NT antibodies linger for many years and decades following infection. Immunoglobulins are not protective.
- Cell-mediated immunity plays a crucial role in disease control and resolution. Virus-specific T lymphocytes prevent the spread of viruses by triggering the lysis of infected reticuloendothelial skin cells.
- A smallpox infection provides complete immunity against reinfection. Vaccination confers immunity that lasts for around ten years. The virus Variola causes smallpox, which is now extinct.
Smallpox
- The duration of incubation varied between 10 and 14 days.
- The prodromal phase, which corresponded to the viremia phase, appeared first. Onset of illness was abrupt.
- The symptoms included a quick onset of fever, severe headache, nausea, pharyngitis, general malaise, and backache.
- In the later stages of the prodromal phase, the palate, tongue, and pharynx would develop an exanthematous rash.
- In contrast to chickenpox, the smallpox rash is characterised by skin lesions that are in the same stage of development.
- The lesions of varicella appear in waves and at different stages, including vesicles, pustules, and scabs.
- The lesions occur initially on the face and extremities before spreading centripetally to the trunk.
- During the course of approximately 17 days, these lesions progress from macules to papules, vesicles, pustules, and then crusts.
- The wounds heal with the production of distinctive scars. Toxemia was the most common cause of mortality in patients with smallpox.
- Two types of smallpox existed: variola major and variola minor.
- The fatality rate linked with variola major was 25–30%, whereas the fatality rate related with variola small was less than 1%.
- In addition, flat smallpox and hemorrhagic variola were uncommon forms of smallpox that were typically fatal in some patients.
Epidemiology of Variola (Smallpox) Virus
Geographical distribution
- Somalia recorded its final incidence of naturally occurring smallpox in 1977.
- The last human case, which was the result of an accidental laboratory infection, was reported in 1978 in England.
- In 1980, the WHO declared that smallpox had been eradicated from the planet.
- Currently, the only known viral isolates are stored in the laboratories of the Centers for Disease Control (CDC) in the United States and the Vektor Institute in Russia.
- However, it was discovered in the 1990s that the smallpox virus was exploited by various nations in their biological warfare programmes.
- It is unknown how many countries’ laboratories still contain the virus.
Reservoir, source, and transmission of infection
- Smallpox was an extremely contagious disease.
- The most common sources of infection were respiratory secretions and exudates from the skin lesions.
- The disease was most frequently transmitted by inhaling respiratory droplets from patients with smallpox.
- Once fever began, the individuals were highly contagious during the first week of rash.
Laboratory Diagnosis of Variola (Smallpox) Virus
- Typically, smallpox was diagnosed clinically. Principal diagnostic criteria for smallpox included a feverish prodromal phase occurring 1–4 days before the start of rashes.
- Skin lesions characteristic of smallpox (deep, hard, spherical), which may be umbilicated or confluent.
- Lesions of the skin at the same developmental stage on any area of the body.
Specimens
- Lesions on the skin, such as vesicular fluid, were the preferred specimens.
Microscopy
- If accessible, an electron microscope was utilised to directly demonstrate typical viral particles in clinical specimens.
- It was useful to distinguish a smallpox virus from a chickenpox virus.
- The characteristic eosinophilic inclusion bodies of Guarnieri can be observed under a light microscope in a stained preparation of clinical specimens.
Isolation of the virus
- Viruses are isolated in the laboratory through injection of embryonic chicks and cell cultures.
- This is required for the quick and precise identification of poxvirus infections.
- Embryonated egg: Inoculation of vesicular fluid into the chick embryo’s central apical membrane (CAM) is a reliable method for detecting and identifying variola virus. After 48–72 hours following inoculation, the virus creates distinctive pocks. Vaccinia pocks are huge with necrotic centres, whereas variola pocks are smaller with necrotic centres. The monkeypox and cowpox cause well-defined hemorrhagic lesions, but the tenapoxvirus, molluscum contagiosum, and Parapoxvirus lack CAM growth.
- Cell culture: For viral isolation from clinical specimens, human and nonhuman primate cells, such as monkey kidney and HeLa cells, are employed in cell culture. Viruses are identified by the presence of Guarnieri bodies, the variola virus’s hallmark CPE. In contrast to the vaccinia virus, which produces CPE within 24–48 hours, the variola virus produces CPE relatively slowly. Tenapoxvirus and parapoxvirus grow poorly in cell cultures, but molluscum contagiosum does not grow at all.
Serodiagnosis
- To confirm a diagnosis of poxvirus infection, serological tests were useful.
- The indirect immunofluorescent antibody test as well as the HI, CF, and NT tests are available for demonstrating the presence of serum antibodies after the initial week of infection.
Features of the smallpox that contributed to its total eradication
- Due to the availability of an efficient vaccine, smallpox was the first illness to be eradicated by immunisation campaign.
- A smallpox vaccination that was safe, stable, inexpensive, and simple to administer was available.
- The presence of a scar signified successful smallpox immunisation.
- Due to the fact that there was only a single serotype of the variola virus, vaccination protected against all cases of smallpox.
- Poxviruses infecting humans and other animals share antigenic determinants. Vaccines made from poxviruses isolated from animals could also be used to protect humans.
- Smallpox demonstrated a tight host specificity for humans. Only humans were infectious reservoirs. There were no animal reservoirs or vectors implicated.
- Due to the consistency of the clinical signs of smallpox, cases may be easily identified and diagnosed.
- These aided in the discovery of human instances of smallpox and the adoption of preventative measures to stop the spread of the disease to other susceptible human hosts.
- Subclinical infections did not develop, and neither did chronic viral carriage. The source of infection was a patient with smallpox who was easily identifiable and treatable in the community, and preventative measures were taken.
Treatment of Variola (Smallpox) Virus
- No particular antiviral medicines are available against variola virus.
- Methisazone has some efficacy against certain poxviruses.
- It is solely advised for chemoprevention, not treatment.
- Except for post-vaccination encephalitis, Vaccinia immune globulin is suggested for the treatment of all problems.
- Even though smallpox has been eradicated globally, there is still anxiety about its probable reappearance through bioterrorism.
Prevention and Control
- The first illness to be eradicated by a successful immunisation campaign was smallpox.
- Even before the turn of the first millennium, India and China employed empirical smallpox preventative techniques.
- In the seventeenth century, the technique of variolation involving purposeful injection with virulent strains of variola to avoid variola infection expanded from India to the Old World and then East Europe.
- Variolation became immensely popular throughout Europe until Jenner’s introduction of vaccination in 1796 rendered it obsolete.
- Those that were vaccinated were granted lifetime immunity as a result of the mutation.
- It was a dangerous technique and was associated with a mortality rate that was around one-tenth that of those with a natural disease.
- Furthermore, after variolation, injected individuals were able to transmit smallpox to susceptible individuals for a period of time.
- In the 1960s, the WHO developed a plan for the global elimination of smallpox.
- The disease was then prevalent in 44 nations, with an annual incidence of around 10 million cases worldwide.
- In 1977, when the last instance of endemic smallpox was discovered in Somalia, the illness was eradicated by the use of a very effective and stable vaccine, rapid identification of outbreaks, and ring vaccination of all contacts of an affected individual (see to the box titled “Vaccine”).
References
- Baxby D. Poxviruses. In: Baron S, editor. Medical Microbiology. 4th edition. Galveston (TX): University of Texas Medical Branch at Galveston; 1996. Chapter 69. Available from: https://www.ncbi.nlm.nih.gov/books/NBK8364/
- Smith, G. L., Beard, P., & Skinner, M. A. (2008). Poxviruses. Encyclopedia of Virology, 322–330. doi:10.1016/b978-012374410-4.00691-9
- Buller, R. M. L. (2017). Poxviruses. Infectious Diseases, 1452–1457.e1. doi:10.1016/b978-0-7020-6285-8.00170-2
- Burrell, C. J., Howard, C. R., & Murphy, F. A. (2017). Poxviruses. Fenner and White’s Medical Virology, 229–236. doi:10.1016/b978-0-12-375156-0.00016-3
- Richter, J. (2017). Poxviruses. Tropical Dermatology, 152–165. doi:10.1016/b978-0-323-29634-2.00013-4
- Craighead, J. E. (2000). Poxviruses. Pathology and Pathogenesis of Human Viral Disease, 365–380. doi:10.1016/b978-012195160-3/50027-3
- Poxviridae. (2017). Fenner’s Veterinary Virology, 157–174. doi:10.1016/b978-0-12-800946-8.00007-6
- https://www.sciencedirect.com/topics/medicine-and-dentistry/poxviridae
- https://emedicine.medscape.com/article/226239-overview
- https://www.britannica.com/science/poxvirus
- https://www.cdc.gov/poxvirus/index.html#:~:text=Poxviruses%20are%20brick%20or%20oval,skin%20nodules%2C%20or%20disseminated%20rash.
- https://www.cdc.gov/poxvirus/diseases.html
